Two Approaches to Transforaminal Epidural Steroid Injections for the Treatment of Radiating Low-back Pain: What is the Evidence?
Point/Counterpoint
Guest Discussants: Steven P Cohen, MD, Michael B Furman, MD, MS,
Nicholas H Weber, DO<
Feature Editor: Jaspal Ricky Singh, MD
Low-back pain is common. In fact, up to 80% of us will experience this pain. The lower back is a complex network of spinal muscles, nerves, bones, discs or tendons in the spine. An irritation, problem, or damage to any of these parts may cause pain in the lower back that often travel to other areas of the body. Fortunately, lower back pain often resolves itself and many find that their pain improves with simple treatments.
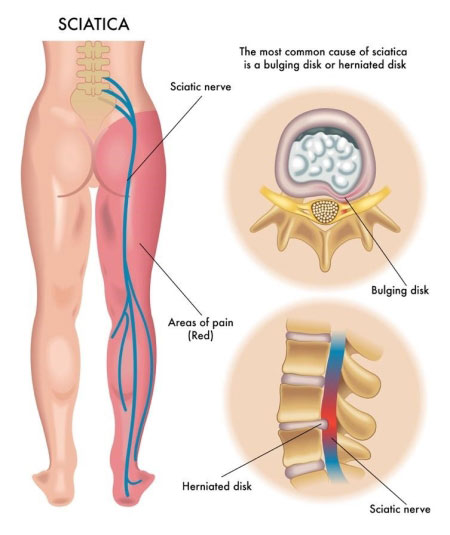
The most common type of low-back pain originates in the lower back and travels through the buttock and down the leg. This is known as lumbosacral radicular pain or sciatica.
Sciatica is most likely to develop around age 40 or 50. Sciatica causes the sensation of pins and needles, a decrease in motor function, or difficulty performing certain movements that decrease one’s activity level and quality of life.
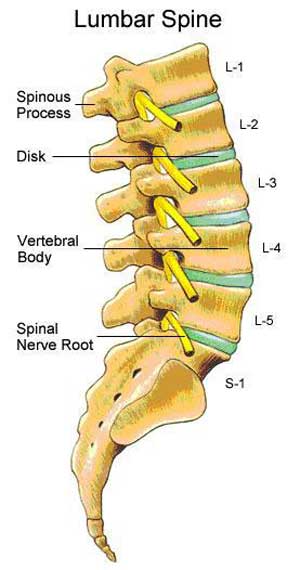
Anatomy of the spine
To understand the cause of sciatica, it is important to understand the anatomy of the spine. The spinal cord can be divided into segments—or levels—according to the nerve roots that branch off. Nerve roots run through the bony spinal canal. In the lumbar and sacrum regions of the spine, a pair of nerve roots exits from the spine at each level.
Spinal stenosis, a narrowing of the disk space, and disk protrusion (also known as a herniated disk) can cause pinching, irritation, and inflammation of the nerve root(s). As a result, people with one or more of these conditions experience low-back pain that can travel to their legs.
To better understand the cause of a patient’s back pain, physicians will perform a physical examination and offer diagnostic tests, such as magnetic resonance imaging (MRI) and electromyography (EMG). The information gathered helps physicians determine the extent of the nerve damage, source of the pain, and determine a plan for managing pain.
Treatment options include lifestyle changes, physical therapy, oral anti-inflammatory or steroid medications, and epidural steroid injections (ESIs).
There are several methods for delivering ESIs, including:
- Interlaminar ESI: An ESI delivered through the back of the spine in the space between two vertebrae and delivering the steroid over a wider area
- Transforaminal ESI (TFESI): An ESI delivered into the opening at the side of the spine where a nerve root exits the spinal cord, allowing for more concentrated delivery to a specific nerve (TFESIs are also referred to ask “nerve blocks.”)
- A single-level TFESI targets the nerve roots that lie across a particular level of the spine causing pain
- A two-level TFESI (or multilevel TFESI) targets two levels of the spine causing pain
In the August 2015 edition of Pain Management and Rehabilitation Journal, three physicians shared differing opinions about single- versus two-level transforaminal epidural steroid injection for alleviating lumbosacral radicular pain. A patient’s case is presented here, followed by a debate as to the best treatment plan. Drs Michael Furman and Nicholas Weber advocate for a 2-level TFESI, while Dr Steven Cohen asserts that a 1-level TFESI is sufficient.
Patient case
Matthew, a 58-year-old man, has been experiencing low-back pain for the last 12 weeks. The pain spreads to his groin, right buttock, and entire leg, causing tingling and numbness.
During Matthew’s physical examination, the physician finds that he experiences pain when he raises his straight right leg. Matthew has full range of motion of his hip, with no pain, and his sensory and motor examination results are normal. However, his knee and Achilles reflexes are worse than normal.
An MRI of his low back indicates mild to moderate stenosis at the L4-L5 and L5-S1 region of his spine, as well as a herniated disk at L5-S1 that is pressing the right S1 nerve. An EMG of his right leg was normal and showed no evidence of nerve damage.
After a trial of physical therapy and oral anti-inflammatory medications, Matthew received an interlaminar ESI that provided significant improvement for 4 to 5 days. He is now frustrated that the pain has returned and requested one more injection before considering surgery.
Steven Cohen, MD, offers his opinions and proposed treatment plan
Before examining Matthew’s specific treatment plan, let’s look at the big picture. Back pain is increasingly common. An estimated 9 million ESIs are performed annually in the United States alone, which means that this is the most common procedure performed at pain management clinics.
We are seeing negative consequences to the high prevalence of ESIs, as the rates of back pain, expenditures, disability rates, and spine surgery have increased steadily. In short, there are significant costs and risks to ESIs, which warrant closer study.
The Food and Drug Administration recently held a panel examining the efficacy of ESIs. Medicare and Medicaid have reduced reimbursement for these procedures sharply. The pain medicine community is reevaluating how we can limit the number of ESIs given and administer them only to the patients who will benefit from them.
The results of a systematic literature review and the guidelines espoused by multiple organizations, including the American Academy of Physical Medicine and Rehabilitation, conclude that no evidence exists to support routinely performing multiple injections.
We as a profession must find the courage to exercise self-restraint in selecting patients to receive ESIs and use the available evidence to determine the proper treatment plan and intervention. We must educate patients that ESIs typically provide relief for less than a few months. Lifestyle changes and physical therapy must be the cornerstone to any plan for managing back pain, not recurring injections.
Matthew received an interlaminar ESI, which provided very short-term relief. A TFESI is an available option now, but what is known about TFESIs? Randomized, controlled trials have shown that single-level TFESIs are effective. Multilevel TFESIs, however, have not been studied in this same way, so there it’s not certain that they are effective. Also, TFESIs administered to the lower back (both single-level and multilevel) carry a risk for catastrophic complications, including death and paralysis. Due to this risk, TFESIs should be administered judiciously.
To improve Matthew’s quality of life, I believe that we as physicians should treat his symptoms. He experiences pain in his thigh, groin, and buttock, which may come from degenerated disks, facet joints, or muscles. Unfortunately, Matthew’s MRI does not clearly indicate which nerve root levels are damaged and causing this pain.
His radiculopathy may or may not be the result of damage to one or more spinal nerve root levels. Multilevel disease is common, occurring in approximately 40% of people with radiculopathy and even more among his age demographic.
Multilevel TFESIs are intended to treat multilevel disease, but studies have shown that a well-placed single-level TFESI spreads the injectate across 2 different spinal levels, effectively achieving this goal.
Studies also indicate that higher dosages of steroids do not improve treatment results. In fact, a randomized controlled trial by Kang et al comparing different doses of steroids of TFESI found that 10 mg of particulate steroid (triamcinolone) may provide maximal benefit.
For Matthew—and the vast majority of back pain patients—I recommend treating in an incremental fashion, starting with conservative options and progressing to more invasive interventions.
The fact that Matthew obtained significant, albeit short-term, relief after the injection suggests that the interlaminar ESI injectate reached the diseased area(s). Moreover, there is more evidence supporting the efficacy of single-level TFESIs than multilevel TFESIs. It is also the more conservative option. For these reasons, I believe the best course of action is to administer Matthew a single-level TFESI.
Michael B Furman, MD, MS, and Nicholas H Weber, DO, respond
When treating back pain, it is very difficult to determine the exact origin of the pain. Physicians cannot diagnose using either symptoms or imaging (MRIs and EMGs) alone; we must assess both.
Matthew’s case illustrates this challenge well. It is difficult to find the area of the spine causing pain from his physical examination. The positive right straight leg raise test suggests that the pain may originate from multiple nerve root levels.
Likewise, it is difficult to draw specific conclusions from his MRI. It does, however, indicate that the pain originates in the right lower levels of his spine. Matthew’s diagnostic test results show that he does not have actual nerve damage. This suggests that he has a good prognosis for recovery with appropriate treatment.
It is also helpful to evaluate Matthew’s response to previous pain treatment. The interlaminar ESI provided some relief, which suggests that the cause of his pain is in the lower spine. It does not, however, help us determine the exact nerve root level.
Considering all these factors, our first choice is to administer a diagnostic TFEI to better determine the exact location of his source of pain. Matthew’s response to this will help us administer another TFESI to the exact source of his pain.
However, Matthew is requesting that we limit our plan to only one more procedure before seeking surgery, which he perceives as the definitive treatment. Since he is only willing to pursue one more procedure, we want to administer an ESI with the greatest chance of alleviating his pain.
A 2-level TFESI will deliver medication to 2 segments of his spine, increasing the likelihood of delivering therapeutic effects. We suggest a 2-level TFESI at L4 and L5 segments.
We believe a 2-level TFESI is the best treatment option for Matthew right now, without any consideration as to the best course of action if his pain returns in the future. If his symptoms return after achieving significant functional benefit for a substantial period from an initial injection, we would repeat the same 2-level TFESI again. Although only single level TFESIs were investigated, the data from Murthy et al suggest that repeating successful TFESIs yields nearly the same benefit as that of the initial injection.
We suggest the 2-level injection because this is most likely our “last shot” at improving Matthew’s condition and quality of life. This option allows us to concentrate the medication where it will be most effective. If that approach does not provide Matthew with significant pain relief, we can comfortably state that we have no further steroid injections to offer.
KEYWORDS
Dermatome: An area of skin that receives signals from one spinal nerve.
Herniated nucleus pulposus: A herniated or slipped disk, also referred to as lumbar radiculopathy.
Lumbar spine: The part of the spine comprised of five vertebral bodies that extend from the lower chest to the bottom of the spine, L1 to L5.
Lumbosacral: Of or relating to or near the small of the back and the back part of the pelvis between the hips, the lower back.
Neuropraxia: A disorder of the peripheral nervous system in which there is a temporary loss of motor and sensory function.
Radiculopathy: A set of conditions in which one or more do not work properly, resulting in pain, weakness, numbness, or difficulty controlling specific muscles.
Sciatica: A medical condition of pain radiating down the lower back and sometimes the hip and leg.
Spinal nerve: A nerve that carries motor, sensory, and autonomic signals between the spinal cord and the body. There are 31 pairs of spinal nerves, one on each side of the vertebral column.
Spinal stenosis: A narrowing of the open spaces within your spine. This can put pressure on your spinal cord and the nerves that travel through it.
Vertebra: The bones that make up the spinal column. In between each vertebra lies a disk.
References
A complete list of references supporting this article can be found in the original journal article.