What Is Sciatica & How Is It Treated?
Sciatica: What It Is & How It’s Treated
The origin of back pain isn’t always obvious, but sciatica presents a distinctive symptom: pain that radiates from your lower back into the side or back of one or both legs. It may be a sharp pain, a dull ache, or something in between, and it’s often accompanied by numbness, tingling, and weakness in your leg or foot.
Sciatica is very common, affecting millions of people in the U.S. each year. 1
Ahead, you’ll find helpful information and resources about sciatica and how it’s treated. It’s important to understand that sciatica is a symptom, not a disease itself. We explore this and more below.
What Is Sciatica, and What Causes It?
Sciatica is pain that radiates into one or both legs; it is caused by compression of the sciatic nerve. The clinical definition of sciatica is lumbar radiculopathy; lumbar refers to the lower part of the back; radiculopathy is pain, numbness, tingling, or weakness caused by a compressed nerve in the spine. Read more about sciatica symptoms here.
The sciatic nerve is the longest nerve in the body. It starts in your lower back and exits your spinal cord, where it splits into branches that run through your hips, buttocks, legs, and feet. Many conditions can cause sciatica or sciatica-like pain.
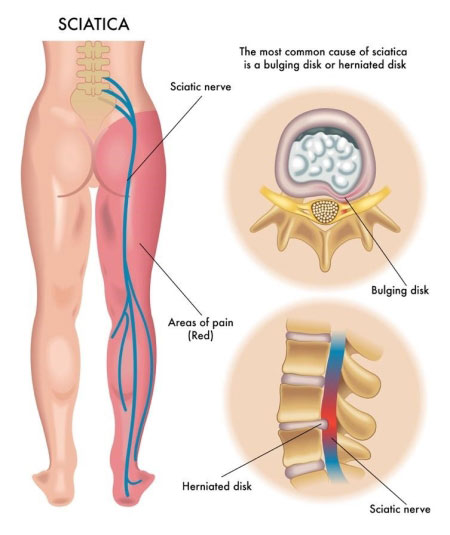
Common causes of sciatica include:
Lumbar Herniated Disc
A herniated disc, also referred to as a ruptured disc, bulging disc, protruding disc, or a pinched nerve, occurs when the gel-like interior of the spinal discs (structures that serve as shock absorbers between the vertebrae) leaks and irritates the nerve; herniation can also happen when the disc becomes compressed from disc degeneration, causing the inner core of the disc to bulge out and press against the nerve. Both cause the shooting pain and other sensations of sciatica. Read more about herniated disc symptoms here.
Note: Many terms are used interchangeably to describe herniated discs, which can be confusing. It’s more important to understand the precise medical diagnosis, which identifies the actual cause of your back/leg/foot pain and other symptoms. To determine the cause of your pain, your spine doctor will review your medical history, perform a complete physical exam, and may order one or more diagnostic tests, as needed.
Degenerative Disc Disease
Degenerative disc disease is a term used to describe the normal changes that occur in your spinal discs over time; the discs tend to dry out (lose fluid) and become flatter and harder due to aging and general wear and tear. Degenerated discs in the lumbar spine can irritate a nerve root and cause sciatica.
Spotlight on AxiaLIF: A Less Invasive Surgical Technique for Degenerative Disc Disease
Spine surgeons can correct degenerative disc disease by fusing together two or more vertebrae and replacing worn discs in the lumbar spine with synthetic replacement material.
Traditional surgical methods to do this call for large incisions in the back or abdomen, which requires complicated dissection of muscles, nerves, and even organs. This puts patients at greater risk of nerve damage and higher blood loss.
Dr. Roger Härtl, the Hansen-MacDonald Professor of Neurological Surgery and Director of Neurosurgery Spine at Weill Cornell Medicine and founder and director of Och Spine at NewYork-Presbyterian at the Weill Cornell Medicine Center for Comprehensive Spine Care, uses a new and less-invasive procedure called AxiaLIF, which involves making only a single small incision near the tailbone.
“AxiaLIF offers another option for minimally invasive procedures for spine surgery and opens up avenues to give surgeons a new way to perform a procedure in a less invasive fashion,” says Dr. Härtl.
The AxiaLIF procedure greatly reduces time in the operating room and is less costly than open surgery. Patients are the main beneficiaries of this minimally invasive surgical technique, enjoying less post-operative pain, shorter hospital stays, and more rapid rehabilitation. Read more here.
Isthmic Spondylolisthesis
Spondylolisthesis occurs when one vertebra slips forward onto the one below it when the bone that connects the two joints becomes fractured. It most commonly occurs at the lowest level of the lumbar spine (the L5-S1 segment). The collapse of the disc space, along with the fracture and the movement of the vertebral segments, can pinch the sciatic nerve, causing sciatica symptoms.
Lumbar Spinal Stenosis
Spinal stenosis refers to leg pain (with or without back pain), which is often aggravated by walking. It is commonly caused by conditions like osteoarthritis, degenerative disc disease, and degenerative spondylolisthesis. Enlargement of the facet joints and herniated discs that put pressure on the nerve roots can also cause spinal stenosis.
Additional problems that can cause sciatica include:
- Spinal tumors, which can compress the sciatic nerve.
- Piriformis syndrome, a disorder in which the piriformis muscle in the buttocks irritates the sciatic nerve.
- Bone spurs, which can put pressure on the sciatic nerve.
- Sacroiliac joint dysfunction, irritation of the sacroiliac joint, which is located at the bottom of the spine; this condition can irritate a nerve that sits at the top of the joint, causing sciatica-type pain.
- Traumatic injury, such as from a car accident or fall.
How Is Sciatica Diagnosed?
Your specific sciatica symptoms can help reveal where the injured or irritated nerve originates. For example:
- Sciatica that originates at the L3-L4 level (see diagram below) in the lower back often includes pain and/or numbness in the middle lower leg and foot; you may also be unable to bring your foot upward (heel walk), and you may have reduced knee-jerk reflex.
- Sciatica that originates at the L5-S1 level (located at the bottom of the spine) may include pain and/or numbness on the outside of the foot and weakness that makes it difficult to raise the heel off the ground or walk on the tiptoes; you may also have a reduced ankle-jerk reflex.
Your spine specialist will review your complete medical history and your symptoms. He or she will also perform a thorough physical exam, which may include things like a straight-leg raise test, during which you will lie on your back with legs straight; your doctor raises each leg, noting the elevation at which your pain begins.
This and other tests can help your doctor pinpoint any affected nerves and help identify disc problems. Your spine doctor may order additional tests, which may include:
- X-rays, which can help reveal herniated discs, osteoarthritis, fractures in the spine, and other problems.
- Magnetic resonance imaging (MRI), which uses magnetic fields and radio-frequency waves to create an image of the spine. An MRI can reveal fine details of the spine, including tumors, nerves, and any damage to the spine. This may or may not be accompanied by a myelogram, which involves injecting a contrast dye into a vein in the patient’s hand or arm during the test; the dye highlights certain tissues and structures and reveals affected nerves.
- A computed tomography (CT) scan, which uses x-rays to create three-dimensional images of the spine and can help reveal compression of the nerves.
Treatment Options for Sciatica
In nearly all (95%) cases of sciatica, simple non-surgical treatments are effective. These include:
- Pain relievers and anti-inflammatory drugs, such as ibuprofen and acetaminophen, as well as steroid injections; oral cortisone can be helpful for mild pain; epidural injections of corticosteroids can help treat severe pain; an epidural works by reducing inflammation of a herniated disc, reducing irritation of the nerve.
- Heat and ice applied for around 20 minutes and repeated every two hours can help alleviate leg pain in the early stages; ice and heat may be alternated, and some people find relief with one more than the other.
- Exercise programs tailored to treat sciatica pain; a regimented exercise plan can help reduce acute sciatica pain and provide conditioning to help prevent future recurrences of pain. Exercise is vital for the health of your spinal discs—the movement helps exchange fluids and nutrients within spinal discs, which can minimize or prevent pressure on the sciatic nerve. Exercises may include walking, stretching, and core strengthening. Your spine specialist will tailor a plan to your specific needs.
Most patients will experience resolution of their sciatica pain with the above measures alone. For the 5% who don’t, surgery may be necessary. Minimally invasive surgical techniques for lumbar radiculopathy include:
- Lumbar laminectomy: Used to treat sciatica pain caused by lumbar spinal stenosis, lumbar laminectomy involves removing the small portion of bone and/or spinal disc material that is irritating the nerve root.
- Microdiscectomy: Involves removing the bulge from the herniated portion of the spinal disc to relieve pressure on the affected nerve. Patients are usually up and walking within a few hours after this minimally invasive procedure, and they generally experience complete or near-complete relief of pain after recovery from surgery.
Read more about surgery for radiculopathy here.
Don’t Suffer from Sciatica—Meet the Experts
The expert spine specialists at Och Spine at NewYork-Presbyterian at the Weill Cornell Medicine Center for Comprehensive Spine Care are committed to providing the highest level of patient-centered care for sciatica, chronic back pain, and the entire spectrum of back and neck conditions.
About Och Spine at NewYork-Presbyterian at the Weill Cornell Medicine Center for Comprehensive Spine Care
Our spine care center is a state-of-the-art clinical facility with 15 doctors across four spinal specialties, including neurology, pain management, rehabilitation medicine, and neurological surgery.
The expert specialists at the spine center take a collaborative approach to care and treat a range of spinal conditions and injuries, from scoliosis to spinal compression fractures to schwannomas (benign tumors). To schedule an appointment with one of our providers, please call 888-922-2257 or use our contact form to send us a message.
Sources
We’ve Got Your Back
For more information about our treatment options, contact our office today.



